- English
- français
Integrated Care: The Centrepiece of Tomorrow’s Health Care System
Editor’s Note: This article is excerpted from a presentation by Medavie Health Services’ President, Erik Sande during the North American Conference on Integrated Care. The October 7, 2021 conference focused on adaptive strategies and change management to build resilient communities and forge new alliances in creating a sustainable healthcare system for the future. It has since been published in the International Journal of Integrated Care.

Across Canada, access to health care is an ongoing challenge. Pressures within our system, including an aging population, chronic illness, hallway medicine and climbing demand have been heightened by COVID-19.
The pandemic has also brought the need to address these challenges with innovative solutions into sharp focus. Enter team-based, integrated approaches to care that create more sustainable paths to help all patients and communities access support — when and where they need it.
Effectively moving care into the community will ensure a stronger future for the health of populations, aligned with “the quadruple aim” of better outcomes, better patient satisfaction, improved provider experience and better cost effectiveness.
An Adaptable, Integrated Approach
Integrated care enables choice. It allows patients to have a voice and actively participate in their care decisions.
It also allows a variety of practitioners to leverage their skillsets to bring care directly to patients in their homes and communities; ultimately increasing capacity in our health systems.
Leaders in our sector helped establish these types of adaptive strategies well before the pandemic. Today, these strategies are being pressure-tested while helping to fill gaps, enhance our ability to deliver health care outside the hospital and bring together dynamic partnerships focused on the health and wellbeing of patients.
What it Looks Like in Practice
Through mobile integrated health (MIH), a highly relevant adaptive strategy, community care teams, including paramedics, nurses and other clinicians (in their homes and through other channels such as telehealth and virtual visits), are working to ease emergency department visits, reduce hospital admissions and expand long-term care options for vulnerable and underserved populations.
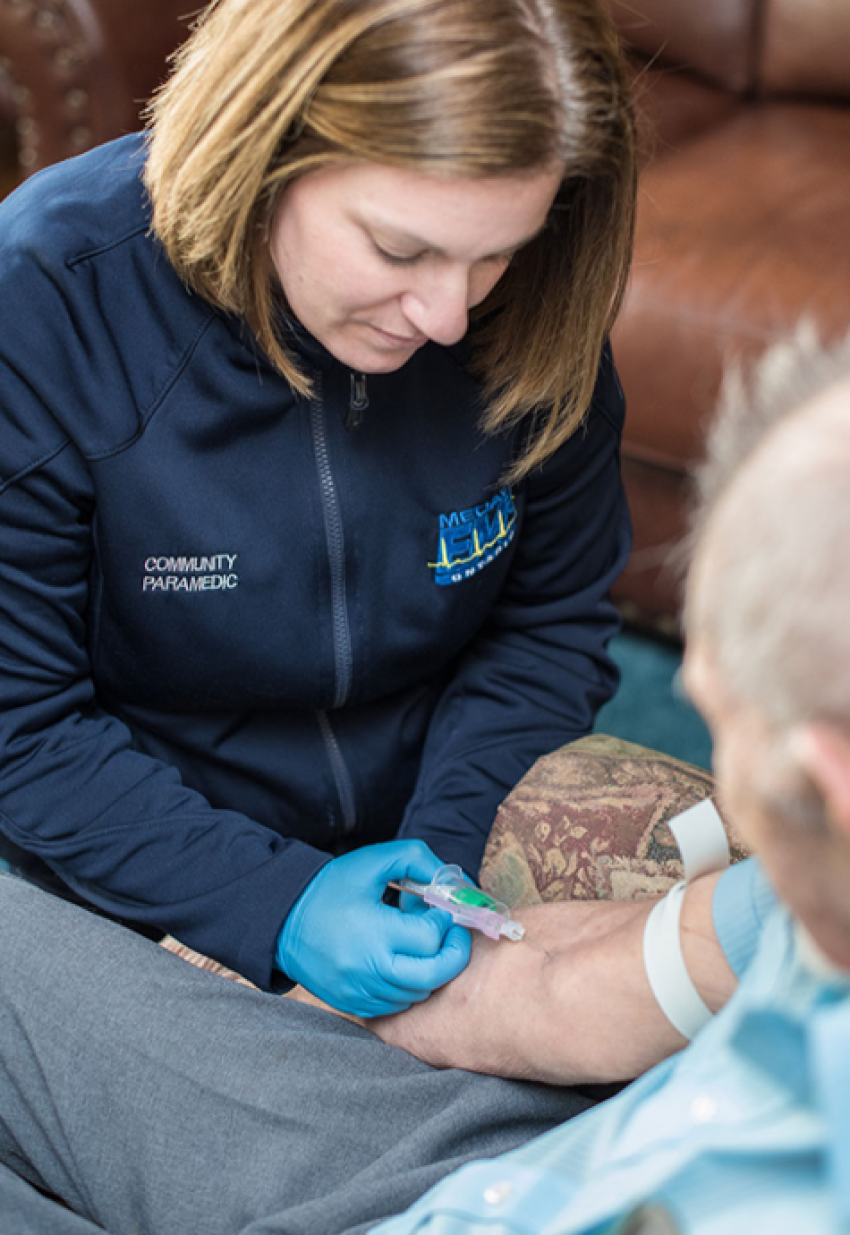
In Chatham-Kent, Ontario, there is a proven MIH model that draws on the skills and mobility of paramedics in the community to provide direct patient care and consultation beyond hospital walls. This is allowing paramedics to provide ongoing monitoring of changing or escalating conditions, perform testing procedures and blood analysis and treat for minor ailments — with proven results.
Additional funding is helping expand the community paramedicine program to support patients on long-term care wait lists and other clinically complex patients, locally.
Evaluations show an 84 per cent reduction in 911 calls and 51 per cent reduction in emergency department visits for targeted populations.
Today’s Change, Tomorrow’s Future
During COVID-19, paramedics have been mobilized across Canada to conduct swab testing (at LTCs and mobile drive-thru clinics) and are engaged in vaccine roll-out and administration, working with local health system partners.
Paramedics are also providing surge capacity response to remote Indigenous communities in northern Canada.
At the Core
Our collective pandemic experiences have reaffirmed what we’ve always known.
We must prioritize integration and delivery of health care outside the hospital, both in rural and urban settings. And, we have to continue to adapt to ever-changing environments and form new alliances. Otherwise needed change will come to a standstill.
Filed under Business Leadership Medavie



